In my days at the hospital I have been focusing on improving services in the special care nursery. Finding alternative ways of feeding babies who cannot breastfeed is vital. With minimal equipment and staff with no specialist skills in caring for premature and sick babies, feeding and kangaroo care are the main things we can do. I described this in an earlier post https://yourmidwife.org.uk/blog/kangaroo-care-for-premature-babies/
Although I have seen formula milk on sale in Malawi, it is rarely used. Without a reliable source of clean water to mix it and a safe way to prepare and give it to a baby, it is not a realistic choice for feeding babies. In the UK we know that formula fed babies are more likely to develop gastroenteritis than breast fed babies https://www.uhsussex.nhs.uk/resources/making-the-choice-to-bottle-feed-your-baby/ A factor in this which isn’t commonly understood is that formula milk once the pack is opened, can very easily become contaminated with bacteria. Scalding the powder with boiling water as you start to mix it can reduce this risk, but this is different to the way that many people mix formula. The formula feed preparation machines are of concern to many health professionals because they do not always heat the initial burst of water to a high enough temperature. There is more information here https://www.feeduk.org/using-a-formula-prep-machine. In Malawi, clean safe water is not always available and there is no way to boil water in the hospital.
In Malawi, choices for feeding babies are much more limited than the privileged choices we have in the industrialised world. I have conflicting feelings about whether this is good or bad. Women here simply know that babies have to be breast fed – and so they do it. I haven’t yet met a single woman who had had a problem with breast milk supply – and many of these women are poorly nourished themselves. The biggest difference in feeding babies here is that no-one pays any attention to clock time! Many women I have met simply can’t tell the time. They also hold their babies most of the time, and carry them with them everywhere. If a baby stirs it is given the opportunity to suck, however recently it last did so. This works beautifully for well, term babies.
It has been important for me to understand what is normal here as I seek to develop the special care nursery. The concept of waking babies for feeds is difficult for many women to accept, but is often essential for sick or premature babies. Then comes the problem of telling the time…..
Numeracy here in Malawi is poor. The education system means that (in theory) children have free access to primary level education. Access to secondary education requires passing assessments and then has to be paid for. However, some primary schools are strict in requiring uniform to be worn – a major problem for many to afford. Most people buy their (very few) clothes from the markets. These markets are where they sell the clothes that we put in charity bins in the UK. Children have to walk to school, often long distances. Now, as the rainy season starts, school attendance will drop. Class sizes are huge, with 80-100 children in a class being commonplace.https://rippleafrica.org/project/education-in-malawi-africa/ With a single teacher, this obviously means that individual attention and help is rarely possible and it is extremely difficult for teachers to check pupil’s understanding. I have been shocked to realise that even professional healthcare staff often struggle with numeracy issues. When a baby needs to be fed every 3 hours, and last fed at 11am, many staff have to actively stop, think and then count, to work out the time of the next feed (not always correctly).
This has presented a number of challenges. I have been troubled by the idea that it might appear that I am being condescending towards people here when I simplify explanations or offer prompts, but then I have found that no offence at all is taken. An example is that I have installed a simple clock in the nursery (sourced from the UK as I couldn’t find one here). In order to ensure that these vulnerable babies are fed appropriately I have marked feed times for every 2 hours in red and every 3 hours in blue. This means a simple instruction, for both staff and mothers, that every time the hour hand reaches the relevant marker, it is time for feeding babies. I have found it possible to explain this by sign language alone (the multiple languages here are impossibly challenging for me). This also has the benefit that a nurse/midwife can observe and help with several babies feeding simultaneously. I had found that because breast feeding is universal it is simply assumed that every mother:baby dyad are doing it effectively.
Putting a baby to the breast is not the same as effective latching, sucking and swallowing. A tiny or sick baby often doesn’t have sufficient energy to suck well. When I arrived I was told that cup feeding of expressed breast milk is used for premature babies, but it has become clear that staff had very little idea of the way to implement this safely. They also didn’t understand how to calculate how much expressed breast milk needs to be given at each feed.
In the industrialised world, we routinely use tube feeding for premature or sick babies. Whilst I have now found some tubes in the storeroom at the hospital, unless staff know how to insert and use them safely this remains something which cannot be done here. Ensuring that every member of staff is safe and competent is not going to be possible in the time I am here. It seems extreme that a baby needs to be transferred to the regional hospital for this alone, but I am not willing to knowingly introduce a practice which could be very dangerous. The big problem with tube feeding is the risk that the tube is misplaced, so that milk is directed into the lungs rather than the stomach. In the UK we check the positioning of the tube (and that the previous feed has been absorbed) by attaching a syringe and checking the liquid obtained with litmus paper. Stomach acid will turn the paper red. If there is any remaining doubt an X-ray can be used. Neither of these options exist here.
This week, we had a premature baby who really wasn’t mature enough to suck. She was estimated to be around 32 weeks gestation. In all discussions about feeding babies it is generally accepted that ingesting colostrum in the first hour after birth is very important. This faced us with a challenge. Baby had no interest in latching at the breast and showed little sucking reflex when I inserted a gloved finger into her mouth. This was a time for fingertip feeding – something my Malawian colleague had never been shown how to do. The mother was able to express a little colostrum and I showed her how to dip her (freshly washed) finger into it and then to apply initially to her baby’s lips. As her baby started to respond, with minimal mouth opening & licking, she was able to insert her finger repeatedly, allowing time for her baby to feel and deal with the tiny amount of liquid transferred each time. Touching a baby’s lips, tongue and roof of the mouth will lead a healthy term baby to suck, but in a premature baby this takes time to develop https://www.healthline.com/health/parenting/sucking-reflex#reflexes Co-ordinating swallowing, making sure that the milk goes down the right way (into the stomach not the lungs) takes time and practice for babies. Nature is wise enough that only tiny amounts of colostrum are needed on the first day of life, so allowing babies time to practice before the quantity of milk and flow rate increase. This is something that almost all new parents need reassurance about during early breastfeeding.
Getting a suitable pot to use is a challenge, but I managed to find a few in the hospital lab. They are not perfect, but they are better than nothing. Once I am back in the UK I will try to arrange to send a case to my colleagues here.
Over the course of the week, we have watched this baby’s interest and ability develop. Finger feeding is very time consuming. An option can be syringe feeding, but the risks of squirting milk faster than baby can cope with it and so leading to choking, means that I am reluctant to suggest this to any but the most well informed staff or parents. Baby is now starting most feeds as finger feeds and then taking some by cup. Watching her little tongue stretch out to draw the milk from the cup for the first time, followed by a big gulp was cause for celebration with the mother!
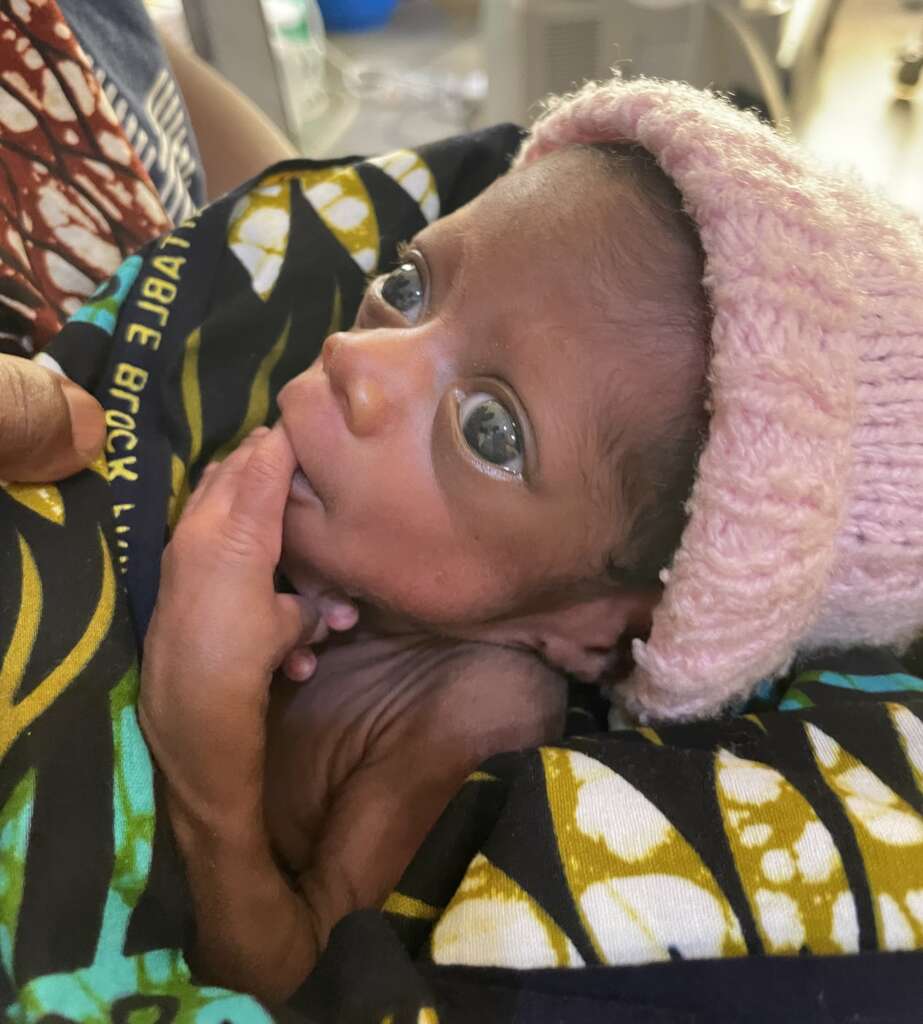
For those who are wondering, the tiny baby featured in my previous post was discharged home this week after 37 days in the special care nursery. We have done nothing other than advise about kangaroo care and feeding. She now weighs 1200g (2lb 10oz). I will be meeting them at their local clinic once a week until I leave to monitor her weight and to recalculate the necessary volume for cup feeding. She is sucking at the breast a little now and I expect that to develop in the next few weeks so that we can reduce the cup feeds. This baby’s survival is absolutely astonishing and in very large part due to her mother’s absolute commitment. She sat or lay on the concrete floor of the nursery for 37 days, feeding her baby expressed breast milk by cup every 2 hours. I am honoured to have been part of their story.


1 Comment
Feeding the baby every 2 hrs for 37 days , sleeping on a concrete floor says it all, love, resilience , strength, determination, survival instinct . Incredible ! xx